Unveiling a New Brain Culprit Behind High Blood Pressure
Scientists have identified a previously overlooked region in the brainstem that may play a significant role in the development of high blood pressure, commonly known as hypertension. This discovery potentially opens new avenues for understanding and treating a widespread chronic condition affecting millions globally.
The focus of this research is the lateral parafacial region, a cluster of nerves nestled within the brainstem. This area is already known for its involvement in regulating essential automatic bodily functions, including digestion, respiration, and heart rate. Furthermore, it is activated during activities that involve forceful exhalations, such as laughing, exercising, or coughing, producing the characteristic sounds associated with these actions.
However, a recent study conducted by researchers in New Zealand has revealed a more profound impact of this brain region. Their findings suggest that stimulating the lateral parafacial region can also trigger nerves responsible for constricting blood vessels. This constriction leads to an increase in blood pressure, a key factor in the development of hypertension.
Experimental Evidence: From Lab Rats to Potential Human Insights
In controlled laboratory experiments, researchers were able to meticulously activate and inhibit the nerves within the lateral parafacial region of rats. Throughout these procedures, they closely monitored the animals’ blood pressure. The results were striking: blood pressure consistently rose when the lateral parafacial region was active and subsequently decreased to normal levels when its activity was suppressed.
Dr. Julian Paton, a physiologist at the University of Auckland and the lead researcher on this study, commented on the significance of their findings. “We’ve unearthed a new region of the brain that is causing high blood pressure. Yes, the brain is to blame for hypertension!” he stated. “We discovered that, in conditions of high blood pressure, the lateral parafacial region is activated, and when our team inactivated this region, blood pressure fell to normal levels.”
While the study was conducted on rodents, the researchers acknowledge the need for further investigation to confirm these findings in humans. Developing methods to safely and effectively test the role of this brain region in human subjects will be a crucial next step in validating this groundbreaking discovery.

Beyond Lifestyle: The Brain’s Role in Hypertension
The exact proportion of high blood pressure cases attributable to this newly identified brain mechanism remains unclear. Historically, lifestyle factors have been widely recognized as primary drivers of hypertension. These include dietary habits such as excessive salt intake, prolonged periods of stress, obesity, and immoderate alcohol consumption.
However, a growing body of scientific evidence is increasingly pointing towards a more complex picture, suggesting a significant link between the brain and the development of hypertension. The brain acts as a central control hub, sending intricate signals throughout the body to modulate crucial physiological parameters like heart rate and the diameter of blood vessels, both of which directly influence blood pressure.
The implications of this research are far-reaching. The scientists involved believe their findings could pave the way for the development of novel therapeutic strategies for hypertension. These new treatments might focus on modulating or calming the specific nerve pathways within the brain that are implicated in driving elevated blood pressure, offering a targeted approach beyond traditional methods.
Understanding the Scope of Hypertension
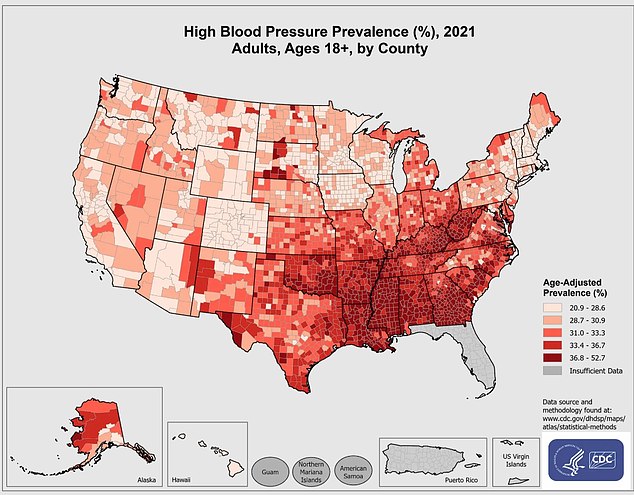
Hypertension is a pervasive health issue, particularly in the United States. According to the Centers for Disease Control and Prevention (CDC), an estimated 120 million adults, representing nearly half of the American population, suffer from this condition.
A healthy blood pressure reading is generally considered to be less than 120/80 mmHg. The upper number, systolic pressure, indicates the force of blood against artery walls when the heart contracts. The lower number, diastolic pressure, reflects the pressure in the arteries when the heart rests between beats. Readings consistently above 120/80 mmHg are classified as high blood pressure.
Medical professionals consistently emphasize the importance of managing blood pressure due to its severe health consequences. Uncontrolled hypertension can inflict significant damage on blood vessels, substantially increasing the risk of debilitating conditions such as stroke, heart attack, dementia, and a host of other serious health problems. The CDC reports that approximately one in six deaths in the US is linked to hypertension, with the condition being associated with 664,470 fatalities annually, accounting for about one in five deaths nationwide.
Current Management and Future Directions
Currently, the primary approach to managing high blood pressure involves medications designed to relax and widen blood vessels, thereby reducing pressure. Complementary to pharmacological interventions, patients are strongly advised to adopt a healthy lifestyle. This includes maintaining a healthy body weight, engaging in regular physical activity, and adhering to a balanced, nutritious diet.
The study published in the journal Circulation Research utilized advanced techniques, employing viruses to either stimulate or sedate the nerves within the lateral parafacial region of the rats. Researchers meticulously tracked neural signals originating from the rostral ventrolateral medulla, a critical area of the brainstem responsible for blood pressure regulation, while simultaneously monitoring blood pressure readings.
The experimental outcomes demonstrated that activating the parafacial region in rats induced forceful exhalations and stimulated the sympathetic nervous system – the body’s ‘fight-or-flight’ response – by constricting blood vessels. Conversely, inhibiting these nerves effectively halted the active expiration and relaxed the blood vessel walls, allowing blood pressure to normalize while breathing continued unimpeded.
This recent discovery builds upon previous research, including a study from the MD Anderson Cancer Center published the previous year. That research suggested a potential link between the hypothalamus, a brain region governing the sympathetic nervous system, and high blood pressure. Their findings indicated that an overactive hypothalamus could lead to elevated blood pressure and an increased risk of heart disease and dementia. That study further explored the role of proteins like calcineurin and RCAN1 in regulating hypothalamic activity, highlighting the intricate molecular mechanisms at play.
The ongoing exploration into the brain’s intricate control over cardiovascular health is crucial. Understanding these complex neural pathways offers hope for more effective and targeted treatments for hypertension, potentially improving the quality of life and longevity for millions worldwide.